News
Making a Difference at Home and Abroad
July 3, 2019
TOP PHOTO: NYITCOM medical students from the Long Island and Arkansas locations mingle with members of the community on their service-learning trip to Ghana.
Studying to be a health professional at NYIT means being committed to making a positive impact on communities around the world. NYIT students get hands-on experience in their chosen fields while volunteering their services and doing good at the same time.
In June 2018, eight NYIT College of Osteopathic Medicine (NYITCOM) students embarked on a service-learning trip to deliver medical outreach to underserved populations in Ghana. Although it was the eighth time NYIT’s Center for Global Health had taken students to Ghana, this trip was special.
Lillian Niwagaba, Ph.D., assistant professor and director of NYIT’s Center for Global Health, introduced her students to Bismark Adu-Appiah, who previously served as the NYIT group’s interpreter in 2012. Now Adu-Appiah himself was a medical student at Kwame Nkrumah University of Science and Technology (KNUST) School of Medical Sciences, a career path he says was inspired by his experience with the Center for Global Health. Getting there wasn’t easy—Adu-Appiah applied to medical school five times before he was accepted. He persevered thanks to former NYITCOM student Jackie Chua (D.O. ’15), M.P.H., who encouraged him to keep trying. “The opportunity of service to others in terms of health fascinated me,” Adu-Appiah says. “I was amazed how much I could contribute to the average Ghanaian.” He reached out to Niwagaba and arranged for the NYIT group to meet with his medical school dean and learn about medical training in Ghana.
That’s what the Center for Global Health is all about, says Niwagaba. “Our global health impact in Ghana is not limited to medical outreach in the hospitals and clinics, but to the people we interact with and meet along the way.”
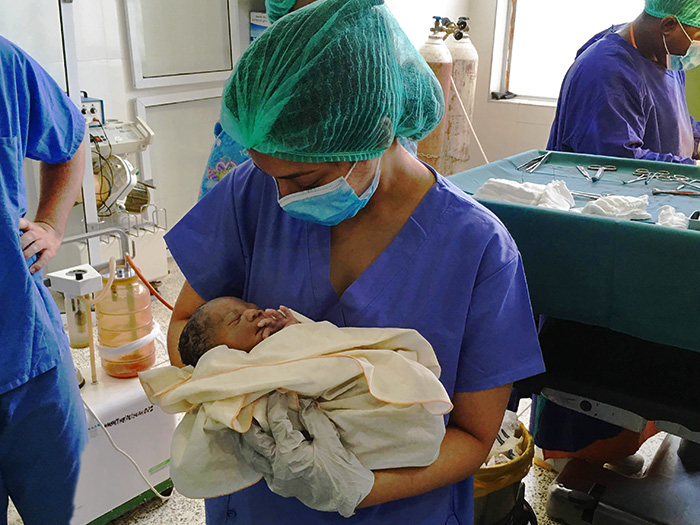
Medical student Anita Thomas holds a newborn at Hawa Memorial Saviour Hospital.
The Center for Global Health is a joint initiative of NYITCOM, NYIT School of Health Professions, and other schools and colleges at NYIT dedicated to developing health-care professionals ready to tackle the global burden of disease and health disparities at home and abroad. The center offers courses leading to a Certificate in Global Health as well as medical outreach programs via trips to Ghana, the Dominican Republic, El Salvador, Nicaragua, Haiti, and Puerto Rico. Over several weeks, students learn about the health system of the country they are visiting, shadow local doctors, offer workshops on public health topics, conduct health screenings, and provide medical supplies and care—all while being supervised by their NYIT preceptors or local doctors.
While the impact on the communities they serve is huge, Niwagaba says the students take away as much as they give. “Students are exposed to medical pathologies and cultures they are unlikely to see at home,” says Niwagaba. “The educational impact is immeasurable—no matter where they serve.”

Medical student Tyler Nghiem demonstrates how to take vitals to school children.
This is true of other programs as well. Last February, Kelly A. Lavin (B.S. ’02), O.T.D., OTR/L, assistant professor in NYIT School of Health Professions, took 12 occupational therapy students on a fieldwork experience to Morocco. The students worked with people of all age groups at clinics across the country including the MAIR Neurorehabilitation Clinic, the only nursing home in Morocco (which also serves as an orphanage), and the King Mohammed VI Rehab School.
The visit came at the invitation of a colleague of Lavin’s, who returned home to Morocco to start its first occupational therapy program. Because there are no licensed occupational therapists in Morocco, Lavin says the need has largely been filled by self-trained volunteers. Her students trained and guided the volunteers and brought supplies and monetary donations they had collected. They raised $1,900 to benefit Clinic Azrou, a privately funded clinic in danger of closing, that provides services to children with traumatic brain injuries and cerebral palsy. Lavin hopes to return in 2020.
“The employees there were not paid and were working out of the goodness of their hearts. The moment they saw the donations, they were all in tears and so were we,” recalls NYIT occupational therapy student Kaitlin Mulhall. “It was amazing to see the effect we had on these people.”

While doing fieldwork in Essaouira, Morocco, occupational therapy students and faculty members had the opportunity to see goats that climb argan trees to eat the nuts
Care Closer to Home
Kanawha County, Charleston, W.Va., is classified as an urban blight area in Appalachia. “The community has a very high rate of substance abuse and obesity,” says Melanie Austin (B.S. ’00), O.T.D., M.P.A., assistant professor of Occupational Therapy.
Last March, she and Zehra Ahmed (B.S. ’04, M.S. ’18), PA-C, M.B.B.S., assistant professor and chair of the Department of Physician Assistant Studies, brought students from the nursing, occupational therapy, and physician assistant (PA) programs to Charleston to learn more about the challenges of working in underserved communities and to help develop solutions.
The students partnered with community leader Pastor Matthew Watts of HOPE Community Development Center (CDC) to conduct interactive workshops addressing the emotional, physical, sexual, social, and environmental health needs for community members of all ages.
They also worked with a group of women living at a halfway house. “It was just amazing and inspiring to see our students connect with these women and empower them to take control over their own health,” says Ahmed, who also serves as assistant director for cultural competency and community education for the Center for Global Health.
The students learned about public health in a way they never could in a classroom. Physician assistant student Tahia Syeda recalls, “I learned how we can target the fundamental beliefs of a community to improve their outcomes—medically, economically, and socially.”
Closer to campus, NYITCOM offers free medical care to uninsured patients through the NYIT Community Free Clinic at the Family Health Care Center in Central Islip, N.Y.
Established in 2016, the clinic is open two Sunday afternoons per month (from 10 a.m. to 2 p.m.) and is staffed by NYITCOM faculty and students. “We are in a unique position to offer a hands-on clinical educational experience for our medical students while also providing a valuable and much-needed service to uninsured residents of the area,” says Sonia Rivera-Martinez (D.O. ’02), associate professor and associate medical director of the Family Health Care Center and director of the NYIT Community Free Clinic.
“The students are involved in all aspects of the clinic,” says Rivera-Martinez. “They register the patients when they arrive, take histories, present the case to the attending, and under supervision, execute the plan of care. They do the documentation in the electronic health record and any follow up with the patient that’s required in terms of blood tests or imaging.”
For patients, the impact of the clinic is also profound. “We’ve seen hundreds of patients,” says Rivera-Martinez. “We’ve also been able to assist a number of patients in getting health insurance, and then they continue to see us at the Family Health Center.”
While the volunteer experience is currently limited to NYITCOM students, Rivera-Martinez hopes to expand it to include students from the School of Health Professions. “Having students and faculty members in health professions working side by side with medical students will create an interdisciplinary and team-based environment for all students to learn a patient-centered model of care,” she says.
Filling the Physician Void
The Mississippi Delta region has some of the lowest number of physicians per capita in the entire nation. That’s why, when NYITCOM decided to expand to a second location, it partnered with Arkansas State University.
“Arkansas ranks near the bottom of health-care outcomes nationally,” says Shane Speights, D.O., FAAFP, site dean, NYITCOM-Arkansas, and associate professor of Medicine. “This school was developed specifically to meet that need and combat the health-care depression of the region.” And Speights hopes not just to increase the number of physicians, but also the diversity of those physicians. That’s a big reason students there selected the National Outreach for Diversity (NOD) program as their first student-led outreach program.
We’re looking to help kids who probably never thought about going to college but are perfectly capable, and with some mentorship, might truly change their lives.
Shane Speights
NOD sends medical students into local schools to provide important public health information and expose youngsters to potential health careers. The NYITCOM chapter specifically targets the most impoverished elementary and middle schools in the region. “We mentor students, exemplifying professional behavior, encouraging the importance of receiving a collegiate education, and inspiring them with the notion that a career within various STEM and medical professions is feasible,” says medical student and NOD co-director Alexis Antonopolous. (The group also teaches Microsociety Magnet School students.)
Another program, held in conjunction with the School of Health Professions, brings high school juniors and seniors to the Arkansas campus to learn about nursing, occupational therapy, physical therapy, speech therapy, radiation technology, ultrasound technology, and medicine.
“We work closely with high school guidance counselors and target kids who would not otherwise have this opportunity,” says Speights. “We’re looking to help kids who probably never thought about going to college but are perfectly capable, and with some mentorship, might truly change their lives.”
Taking Health on the Road
This summer, with more than $800,000 in funding from the U.S. Department of Agriculture, NYITCOM-Arkansas will bring healthcare to underserved and rural populations thanks to the Delta Care-a-Van—a mobile medical clinic. Currently in development, the van will have two exam rooms and state of-the-art telemedicine technology. The plan is to travel to rural communities to provide preventative care services and health education free of cost and without need for an appointment. Patients will receive health education and screenings for untreated chronic conditions including obesity, diabetes, and anxiety and depression.
“We recognize that underserved populations often have difficulty making it to a healthcare provider, so our plan is to bring the resources and education to them,” says Speights. “At the same time, this service will provide valuable clinical training to an army of future physicians and health-care professionals.”

Daniel Parrinello, a second-year medical student at NYITCOM-Arkansas, leads elementary school students through an exercise at a National Outreach for Diversity event.
In addition to their conventional medical studies, all Arkansas-based medical students are required to complete a population health certificate program. The Delta Care-a-Van will provide the opportunity to apply that knowledge. Under the guidance of faculty and trained medical experts, students will conduct screenings and wellness examinations to monitor blood pressure, blood glucose, and signs of mental health conditions. Patients needing additional treatment will be connected to local providers. They can also receive an on-the-spot telemedicine consultation, building upon the college’s mission to be among the first U.S. medical schools to train first-year medical students in telemedicine.
“We plan for all our students to participate in programs like the Delta Care-a-Van at some level,” says Speights. “We believe it’s important for students to start making a difference before they graduate, and this initiative will be a prime example of that.”
By Renee Levy




