News
Brain Therapy: New Treatments for Neurological Problems
July 8, 2019
TOP PHOTO: A participant in Rock Steady Boxing spars against a dummy as a student volunteer demonstrates technique.
With novel, interdisciplinary approaches to care, physicians and health professionals at NYIT are improving the lives of those with neurological disorders and making breakthroughs in the field.

Walk into a Rock Steady Boxing session at the NYIT de Seversky Wellness Gym on the Long Island campus and you’re greeted by the steady thump of fists against speed bags.
But these boxers aren’t training for the ring, they are Parkinson’s disease patients, mostly older adults, involved in Rock Steady Boxing—a unique fitness program designed to help them maintain and improve their motor skills and balance. And their coaches are physicians, students, and other health professionals from NYITCOM and NYIT School of Health Professions.
The program is just one of several areas where New York Institute of Technology is taking a new holistic approach to helping patients with neurological disorders. “Good health is a lifelong goal requiring a variety of specialists working together for the benefit of every member of our society,” says Gordon Schmidt, Ph.D., FACSM, dean of NYIT School of Health Professions. “To achieve that, we work with many disciplines at NYIT and with health professionals in our community.”
Boxing to Find Balance
Approximately 1 million people in the United States have Parkinson’s disease and 60,000 are diagnosed each year, according to the Parkinson’s Disease Foundation. The neurodegenerative disease erodes parts of the brain associated with motor control and patients slowly lose control of their body as the disease progresses.

Adena Leder (center) works with participants of Rock Steady Boxing on the Long Island campus.
“Rock Steady Boxing is a vigorous exercise program for patients with Parkinson’s,” says neurologist Adena Leder (D.O. ’99), director of NYIT’s Adele Smithers Parkinson’s Disease Treatment Center and a specialist in movement disorders. She helped start NYIT’s Rock Steady Boxing program, an affiliate of a national program, in 2016.
And the program goes beyond exercises in the gym. “Improved fitness is only one of our goals for this program,” says Rosemary Gallagher, PT, D.P.T., Ph.D., associate professor in the Doctor of Physical Therapy program at NYIT School of Health Professions. “Parkinson’s disease can be very isolating due to the physical manifestations of the disease. One of our primary goals is socialization, for both our boxers and caregivers.” Gallagher also notes that the program’s interdisciplinary nature (in addition to Leder and Gallagher, staff members include physical and occupational therapists and other specialists) not only helps boxers, but also gives student volunteers the opportunity to learn about related fields.
And research shows it works. According to pilot study results presented at the 2018 International Conference on Parkinson’s Disease and Movement Disorders, patients who participated in the program had faster reaction times than patients who did not. “Reaction time is something that could eventually lead to falling or not being able to drive, which are huge lifestyle changes,” says NYITCOM medical student Christopher McLeod. “[This study] shows how Rock Steady Boxing and exercise programs that use sequences could help slow the decline, or maintain a level of functioning longer, in Parkinson’s disease.”
Medical Foundation
Rock Steady Boxing is an extension of the comprehensive, interdisciplinary care provided by the Adele Smithers Parkinson’s Disease Treatment Center. It also provides medical care along with physical, occupational, and speech therapy services to patients at the Riland Academic Health Care Center.
“We’re the only center in this area that offers specialized therapy in all of those areas in one place,” says Leder. “We know Parkinson’s. Everyone works as a team, and it’s a one-stop shop for our patients. We’re looking for ways to improve the course of their disease and their quality of life.”
One aspect of treatment that sets the center apart is the use of osteopathic manipulative medicine (OMM). According to Sheldon Yao (D.O. ’02), associate professor and chair of the NYITCOM Department of Osteopathic Manipulative Medicine, OMM helps decrease some of the muscle spasm and motor problems that often accompany Parkinson’s disease. One of his studies, published in the journal NeuroRehabilitation, demonstrated that OMM techniques targeting the spine and extremities are effective in helping to improve motor function and balance in subjects with more advanced Parkinson’s disease.
“By using different techniques, we are able to get the muscles to function better and eliminate spasms, which improves patients’ stride and balance,” Yao says. “Because they’re able to ambulate better and are feeling more balanced, they’re able to do more. It really helps with quality of life.
Rare Expertise
The Ehlers-Danlos syndromes (EDS) are a group of connective tissue disorders that can be inherited and are varied both in how they affect the body and in their genetic causes. They are generally characterized by joint hypermobility (joints that stretch farther than normal), skin hyperextensibility (skin that can be stretched further than normal), and tissue fragility.
It’s a rare disease—difficult to diagnose and harder to treat—and specialists are few and far between. Bernadette Riley, D.O., associate professor at NYITCOM and director of the center, says that’s part of what makes the university’s Ehlers Danlos Syndrome and Hypermobility Treatment Center so remarkable.
While 13 of the EDS subtypes have a known genetic association, the focus of the center, hypermobile EDS and hypermobility spectrum disorders, do not. “Our focus is on symptomatic relief of all the comorbidities, including neurological manifestations,” says Riley. These include severe headaches, neck pain, vertigo, and TMJ disorders.
The NYIT EDS/Hypermobility Treatment Center is unique in that it provides necessary care to patients in one setting, including primary care, neurology, occupational and physical therapy, OMM for symptom relief, and cognitive behavioral therapy to help patients cope with their pain. “Our patients really appreciate that all of our doctors are familiar with hypermobility and with the cranial instabilities that can also be present,” says Riley, who is involved in research on various aspects of EDS and hypermobility treatment, including OMM and psychological treatment. “There is a lot of potential to add to the knowledge base.”
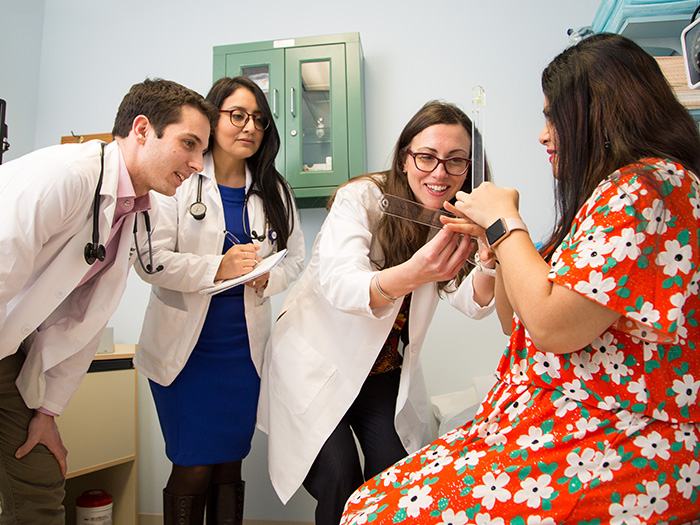
Medical professionals and staff in the NYIT EDS/Hypermobility Treatment Center provide comprehensive care to patients with EhlersDanlos syndrome.
A Physical Approach
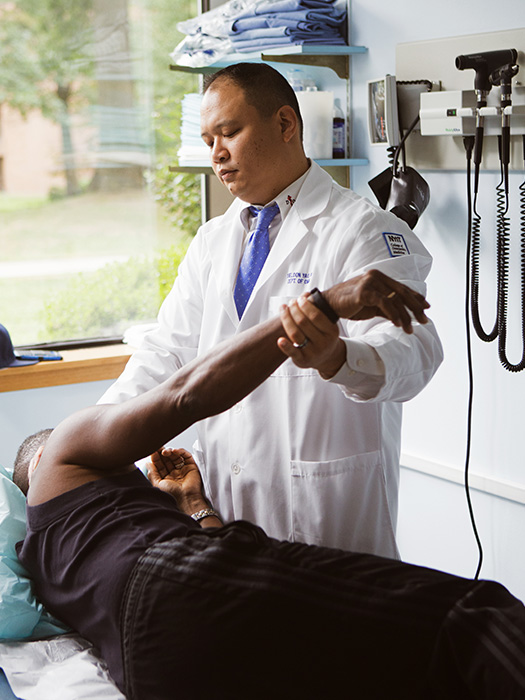
Sheldon Yao uses OMM to help a patient.
Exercise can also benefit young people with neurological disorders such as autism spectrum disorder (ASD). NYIT has joined forces with Inclusive Sports and Fitness (ISF), a Suffolk County-based nonprofit that helps children with developmental and intellectual disorders advance their sensorimotor, social, emotional, and cognitive abilities.
ISF was created in 2013 by Occupational Therapist Alexander Lopez, J.D., now associate professor at NYIT School of Health Professions. “ASD is a disruption in the neural pathway of core processing of information,” he explains. “Patients have difficulty processing information in the brain and can be hyper- or hyposensitive to sensory feedback.” ISF creates activities for individuals that help rewire the brain so that they can perform more typically. “The training that we do is repetitive in nature,” explains Lopez. “It may not be the same every time because we want some novelty, but we try to do repetitive activities that teach participants how to move their bodies more effectively. That creates new neural pathways and learning experiences that can be transferred to other things.”
Lopez says the NYIT collaboration is helping take ISF to the next level. “We’re bringing science and medicine together for the best interests of children and adults with autism,” he says. Eventually, the university hopes to open a center on campus. The program is also highly interdisciplinary. “We all feel there is tremendous potential here,” says Schmidt. “Our involvement as an institution to take this research to the next level is integral to our mission. We want our faculty to gain collaborations across many disciplines.”
Good health is a lifelong goal requiring a variety of specialists working together for the benefit of every member of our society.
Gordon Schmidt
Lopez’s principal NYIT collaborators include Thomas Chan (D.O. ’99), assistant professor of Clinical Specialties; Sara Winter (M.S. ’08), PA-C, M.S.P.A., SLP, assistant professor of Physician Assistant Studies; and Peter Douris, PT, Ed.D., D.P.T., professor of Physical Therapy. It also involves faculty from NYIT College of Engineering and Computing Sciences—Ziqian (Cecilia) Dong, Ph.D., Huanying (Helen) Gu, Ph.D., and Maryam Ravan, Ph.D.— who are incorporating virtual reality into interventions for children with ASD and using electroencephalogram tests to look at brain changes that result from these interventions.
“We’re hoping this unique collaboration makes us more innovative than any other center in terms of service and research,” says Lopez.
Our Students are VIPs
NYIT’s collaboration with the ISF program is a natural, given the institution’s Vocational Independence Program (VIP), a three-year program for college-aged students with mild intellectual disabilities—mostly high-functioning autism—that began in 1987. Students in the program take non-credit classes in executive functioning, social skills and communication, independent living, and employment skills. Each student also has an academic advisor; social counselor; and independent living, job, and banking coaches. The goal is for students to graduate with the skills to live independently and hold a job. “Very few programs provide all of these experiences as well as the individualized social, academic, employment, and financial coaching,” says Paul Cavanagh, Ph.D., senior director of the program.

Students in the Vocational Independence Program take academic classes and develop executive functioning skills.
Associate Professor Kelly A. Lavin (B.S. ’02), O.T.D., OTR/L, an occupational therapist, works with VIP students on executive function, her area of specialty. “Executive functioning is essentially the ability to plan and execute your day—take a shower, go to work, remember to buy dog food. It’s the ability to attend to what you need to attend to and filter out what you don’t,” she explains. Many disorders such as ASD are associated with what she calls “executive dysfunction.”
She is now collaborating with Cavanagh on research to study the efficacy of particular executive function interventions on VIP students. To help them, she has engaged occupational therapy students at NYIT, SUNY Stony Brook, and Touro College to help VIP students with social skills, daily activities, and job searching.
“This is one of the biggest challenges for this population,” she says. “Our goal is to develop an evidence-based intervention model that can really be effective in facilitating changes in our VIP students’ executive function skills.”




